Total Knee Replacement Recovery Checker
Phase Name
Short description.
Walking Aid
Walker
-
Flexion Target✓
Sit and stand safely -
Distance/Mobility✓
Indoor transfers only -
Focus Area✓
Prevent clots
Check for numbness below 90 degrees.
The Reality of Walking After Knee Surgery
If you are asking how long it takes to walk normally after total knee replacement, you likely want a straight answer. The truth isn’t a single number, but a progression. Most patients stand up on their own within 24 hours of surgery. By the time you reach three months, many walk without a cane. However, full muscle balance and a stride indistinguishable from your pre-surgery self often take six to twelve months.
We need to distinguish between simply putting weight on the leg and walking “normally.” Total Knee Replacement is a surgical procedure where damaged knee joint surfaces are replaced with artificial components made of metal and plastic. Also known as Total Knee Arthroplasty, it aims to reduce pain and restore function. The success relies heavily on patient engagement during recovery phases. In 2026, modern rapid recovery protocols mean we discharge patients faster, but your personal journey still depends on your biology and dedication.
Days One to Three: The Immediate Post-Op Phase
You will leave the operating room feeling numb due to nerve blocks. Within six to ten hours, physical therapists visit you. This is the start of Gait Training. You won’t be walking far. You will sit on the edge of the bed, stand up using a walker, and take two steps. Your surgeon expects this early movement to prevent blood clots and lung issues.
Hospital stays vary. In Sydney, typical inpatient duration is one to two nights for uncomplicated cases. Before leaving, you should manage basic transfers: toilet to bed, bed to chair. You will use a walker at this stage. Pain is significant here. Modern medication regimens prioritize opioid-sparing methods to keep you alert enough to move.
- Day 1: Stand with assistance. Sit up fully.
- Day 2: Short hallway walks. Bathroom independence.
- Day 3: Discharge preparation and home safety assessment.
If you struggle to get the knee above 90 degrees flexion by day three, tell your team immediately. This limits functional mobility later.
Weeks One to Six: The Home Environment
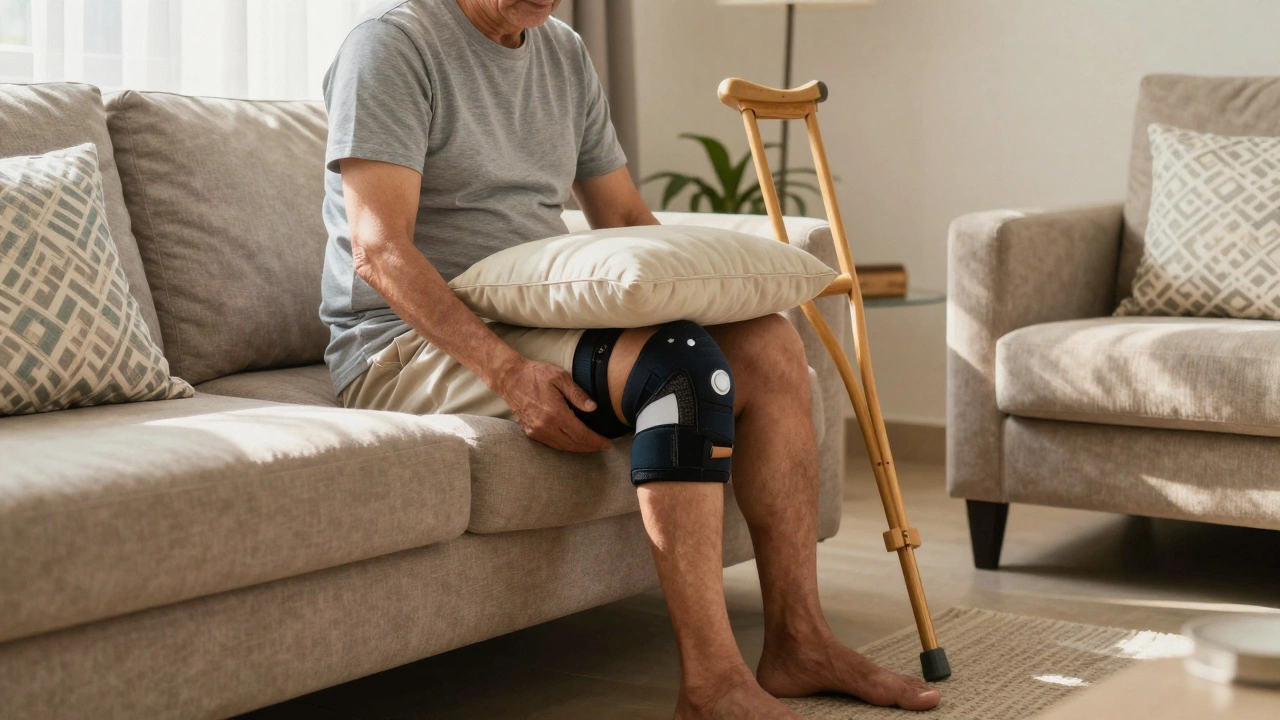
Returning home changes the game. Floor levels and household hazards dictate your safety. During these weeks, you rely on assistive devices. You are technically walking, but it is functional walking, not athletic walking. You lean heavily on the device. Your quadriceps muscle atrophies quickly after surgery, so regaining control is slow.
About week four, you might swap the walker for a crutch or a cane. This transition happens when you can step through without significant limping. Some patients drop aids by week five, others hold on until week eight. Do not rush this. Limping now trains bad muscle memory that lasts years.
Time Period
Walking Aid
Distance
Pain Level
Weeks 1-2
Walker
Indoor only
Moderate-High
Weeks 3-4
Cane/Crutch
House + Yard
Moderate
Weeks 5-6
No Aid / Occasional Cane
Short Outdoor Walks
Mild
Flexion targets matter here. By week six, you should aim for 90 to 110 degrees bend. Without this range, climbing stairs feels impossible, which impacts independence significantly.
Months Two to Four: Regaining Confidence
This period is often called the plateau phase. You walk, but it doesn’t feel right. You might feel a stiff hinge or occasional catching sensations inside the joint capsule. This is scar tissue maturing. Swelling fluctuates throughout the day; it increases after activity and decreases overnight. Ice packs are essential here to control this inflammation.
By month three, most patients stop using crutches entirely in safe environments. You might still use a cane outdoors for uneven terrain. The gait pattern starts to look symmetrical. Your brain recalibrates proprioception-the sense of where your leg is in space-which was confused by the surgery trauma. Balance exercises become crucial now to prevent falls on slippery tiles or wet paths.
Swelling management remains key. Compression stockings might be discontinued around month two, but elevation is still necessary if standing for long periods. Working full-time jobs usually resumes during this window if duties are sedentary. Heavy labor roles often wait until month four or five.
Six Months and Beyond: The Final Stretch
True normalization of gait continues until year one. You might run short distances by month six, though surgeons generally advise low-impact activities to prolong Implant lifespan. Marathon runners usually resume running after nine months. Sedentary individuals often feel done by month six, while athletes continue strength training past a year.
Stiffness can persist intermittently. Morning stiffness lasting less than 15 minutes is normal. Persistent pain or redness beyond six months needs investigation for infection or mechanical failure. The soft tissues around the incision may tingle or itch permanently due to severed nerves. This does not indicate poor healing but nerve regeneration patterns.

Factors Influencing Your Speed of Recovery
Biology varies wildly. A 45-year-old marathoner heals differently than a 78-year-old diabetic. Pre-operative condition determines post-op speed. Muscles that are strong before surgery lose less strength after surgery.
- Age: Younger patients generally regain ROM faster but require stricter protection to avoid overuse injuries.
- BMI: Higher body mass increases load on the new joint, slowing functional progress.
- Pre-hab: Strengthening quadriceps before the knife helps shorten rehab time by weeks.
- Comorbidities: Diabetes slows wound healing; heart issues limit exercise intensity.
Your mental state matters. Fear of falling often leads to protective guarding behaviors that prevent full extension of the leg. Addressing this fear requires professional guidance from physiotherapists who specialize in geriatric or orthopedic care.
The Critical Role of Physical Therapy
Passive waiting yields inferior results. Active rehabilitation drives outcomes. In Australia, you may access services via private health insurance or public schemes depending on eligibility. Sessions focus on strengthening the hamstring, calf, and glute muscles that support the knee. Quadriceps setting exercises-tightening the thigh muscle without moving the leg-are performed daily.
Without consistent therapy, you risk Adhesions forming inside the joint. These sticky bands of tissue restrict motion. Manipulation under anesthesia is sometimes required if range of motion stalls below 90 degrees at four months. Prevention is better than cure, making attendance vital.
Recognizing Complications Early
While most recover smoothly, watch for red flags. Sudden calf tenderness suggests blood clotting issues (Deep Vein Thrombosis). Fever combined with wound heat indicates potential infection. Numbness spreading up the calf could signal nerve damage. Contact your surgeon immediately rather than waiting for the next scheduled appointment.
When can I drive after knee surgery?
If your right knee was operated on, you generally need reflexes free from strong pain meds, usually around 6 weeks. Left knee patients may drive sooner, around 2 weeks, once you can safely brake.
Is limping normal at 3 months?
Mild limping can persist at 3 months due to muscle weakness. However, a heavy limp suggests gait deviation. Consult your physiotherapist to analyze your stride mechanics.
Can I climb stairs independently?
Most patients navigate stairs with a rail by week 4. Full fluency without hesitation takes up to 6 weeks. Always lead with the good leg going up and the surgical leg going down.
Will my swelling ever go away completely?
Significant swelling subsides by 3 months. Minor ankle or shin puffiness can last up to 12 months. This usually improves with evening rest.
What exercises help gait fastest?
Straight leg raises, heel slides, and seated marches are foundational. Mini-squats and calf pumps improve stability. Consistency beats intensity in the first 8 weeks.





Write a comment